A Brief Introduction to Fascia
FASCIA: WHAT IT IS AND WHY IT MATTERS
is a recent book by David Lesondak, which is pertinent to Parkinson’s Disease - indeed, I believe that the material covered in this book is absolutely-need-to-know for anyone affected by or involved with Parkinson’s Disease. Here, David explains and explores the topic of "fascia" with a narrative style, all backed up by the latest science, yet contextualized through more ancient wisdoms, including how, in large part, our "new" understandings simply help to explain why the old was ever true, illustrated with thought provoking diagrams and photographs of the real stuff.
From this book we discover that fascia is essentially the connective tissue which is found throughout our body, wrapping muscles and organs, nerves and bones. Anyone who has ever tried to cut up a raw chicken breast will have encountered the thin, silvery white connective tissue. It turns out this connective tissue is incredibly important and has profound and primary roles in our biological system, health and wellness. This is an “emerging” field in medicine, but has been known about and worked with in other disciplines for a very long time.
The book explains that fascia consists of collagen fibers suspended in a fluid, which together form a "viscoelastic" substance with unusual properties. Fascia can act both as fibrous net, not only able to resist change of shape and sustain tensile forces, but also flow and creep like a viscous fluid.
"The most important thing to keep foremost in mind, at all times, is that the fascial net is one continuous structure throughout the body... as far as the body is concerned, the fascia is all one - one complex, holistic, organ. The 'everywhereness' of fascia also implies that, indeed, it’s all connected and thus is 'connective tissue' ."
This is illustrated in the book, for example, by a photograph of a single, continuous real piece of fascia taken from a dissection of a human body, which still has the tongue attached at one end and the connective tissue of the toes at the other.
David goes on to explain how the hard skeleton of the bones and the soft skeleton of the fascia in the body, form together a very special type of structure. Without the tensile strands of the collagen fibers which make up the fascia, the body would simply collapse. The author explores the profound importance of having this type of structure in existence throughout or bodies, and details how the unfamiliar properties of such "tensegrity" structures means we do need to reconsider so much about what we've been taught about those bodies.
Subsequent chapters of the book explore how universal fascial structures exist everywhere in the body, and really do matter in all the parts: muscles, cells, nervous system, organs, brain, before going on to to briefly describe how to diagnose fascial issues and selected therapies for addressing these. Problems arise when the fluid part of the fascia is too sticky and can't flow, e.g. when the connective tissue becomes dehydrated, and also when the collagen fibers become unaligned or tangled e.g. through chronic stress, injury, infections and trauma. Likewise, therapy is aimed at re-hydrating the connective tissue and restoring the healthy shape and directions of the fibers. Importantly, the fascia has a massive role in chronic pain, because it is where many of the nerves which sense pain have their nerve endings.
The book is full of awe and wonder, including photographs and results from the very latest cutting edge science: as the author admits, due to the blistering pace at which the science of the day is now opening up the worlds of the fascia, his book is already somewhat out of date! David says:
"I was indeed making changes, additions actually, right up to the very last minute. It wasn't that the new science was over-turning the old, but adding to and enhancing the current knowledge base. I want to assure everyone that everything in the current edition is [still] accurate!"
David also explains in the book why this knowledge has not penetrated into the University medical training systems, as of yet. Indeed, historically, fascia was literally considered as throwaway: after a body had been dissected for medical training and anatomy classes, all the parts were returned to the family for proper ritualistic disposal, apart from the fascia, which was generally thrown out as "human waste"! This says all we need to know about the past medical training mindset towards fascia. This is unfortunate, given how the book clearly explains that our fascinating fascial net may be the one part of the human body which makes us who we are or were, more than any other.
In this article we will explore the implications of all this for movement disorders and chronic "muscle" pain, including an intuitive application to my own experience of rigidity dominant form of Parkinson's Disease.
The Catsuit Concept
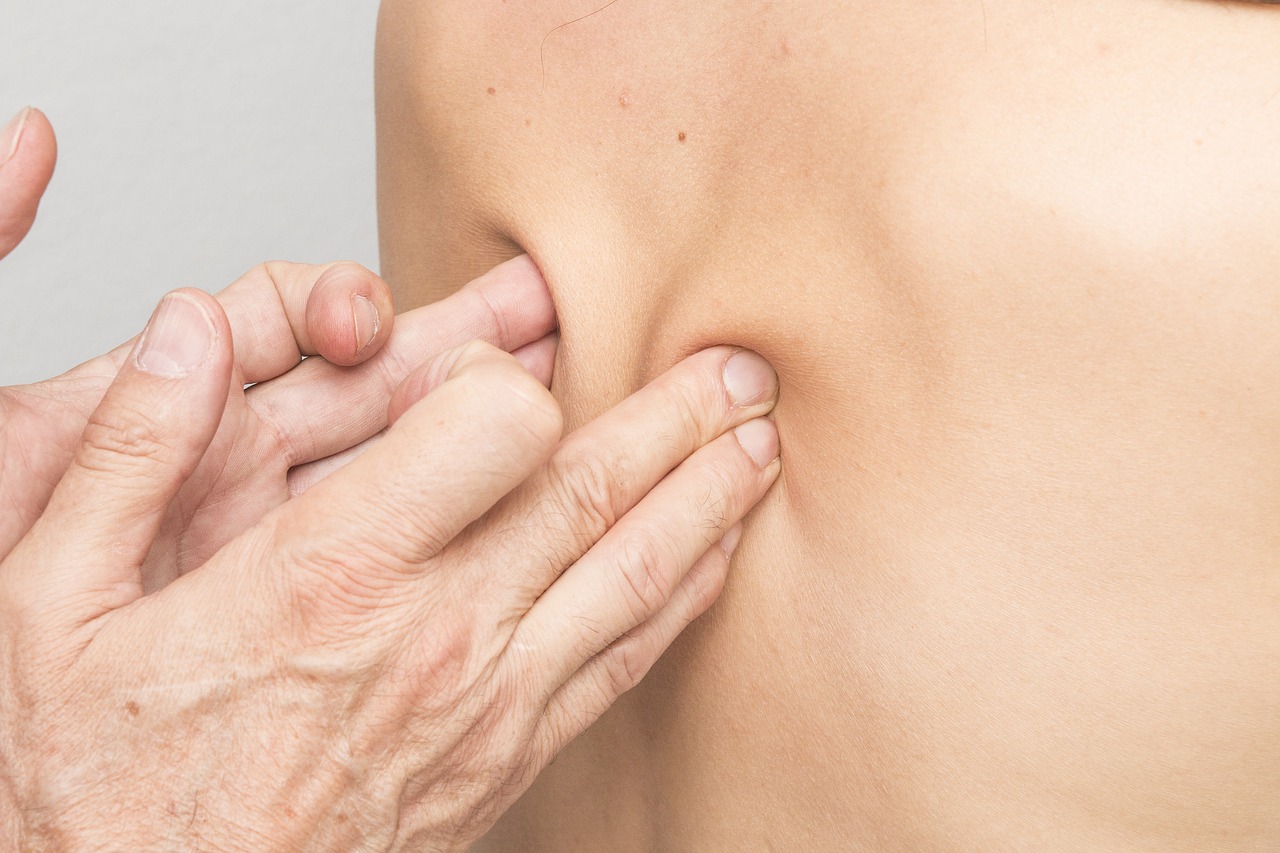
In the book, David describes how the first layer of fascia underneath the skin, called the "superficial" fascia, separates the skin from the muscles, allowing them to slide over one other. The superficial layer also incorporates thermoregulation and lymph and blood flows. Below this is a layer called the deep fascia. It forms discrete pockets around each muscle, and is the silvery white skin one encounters when cutting up a raw chicken breast, for example. It keeps all the muscles separate, helping them slide past one another, yet remain connected and able to communicate with other muscles, remotely, throughout the body.
Envisaging these fascial layers running all through the body reveals a very interesting concept - that we actually have a single piece "full body catsuit" just under the skin, as illustrated in the photo.
This is a profoundly important insight, especially for movement disorders and chronic pain issues, particularly when combined with knowledge that the fascia tends to tighten, contract, stiffen (congeal) in response to stress, via fight, flight, freeze responses, preparing the body for action and perhaps even armouring it in places.
Indeed, given the wealth of knowledge which is rapidly emerging about fascia and its role in our vitality, we do need to consider fascia and incorporate it into our thinking about Parkinson's Disease, other muscle tension issues like dystonia, and chronic pain problems. One very important point to re-iterate is that the sensory nerve endings for signalling pain abound in the fascia itself. If we are missing fascia from our theories of such conditions, I feel that we are missing a hugely important reality, and hence are not likely to arrive at the entirely correct answers.
Returning to the "catsuit" concept, this in itself not only allows me to understand what is going on with my own Parkinson's Disease, but also to be better able communicate what it is like to other people. I can now envisage what is happening, when the dopamine replacement drugs wear off, is that my fascia begins to contract and stiffen again, because, without the drugs, my nervous system is stuck in a profound stress response. Hence the result of drug wear off would seem to me to be just like wearing a shrinking catsuit which becomes too small for my body, and hence is too tight everywhere.
It is easy to imagine how wearing a too small catsuit would result in the legs being drawn up by the toes, the arms being drawn in from the fingers, the head being pulled down forwards or backwards by the hood of the suit, and the shoulders being pulled down and forwards by the tightness of the catsuit there. So, by analogy, I can see how the global tightening/contracting of deep fascia could pull the body into the classic stooped Parkinson's Disease stance. Then, once in this position, making any movement which works against the contraction will be difficult - straightening out the arms or legs, raising or turning the head, raising the shoulders, standing tall with a straight back. Indeed, these are just the types of movement which are hardest for people with PD to do. At the least, I hope the idea helps people to understand what it is like to have PD stiffness/rigidity, by imagining wearing a catsuit which is far too tight!
Symptoms are in the Fascia too?
When talking and thinking about Parkinson's Disease, it is usually in terms of pain and rigidity (hypertension) and stiffness in the muscles themselves. Indeed, no-one in my medical support team has ever even mentioned fascia to me. Yet as we have seen above, our muscles and the fascia which surrounds them are part and parcel of a whole. Indeed, the fascia not only surrounds each muscle, but runs through them, partitioning groups of muscles fibers into bundles, and even surrounds each individual muscle fiber at a smaller scale. Thus, I believe that fascia plays an important role in Parkinson’s Disease symptoms, especially stiffness, pain and rigidity in the body, and it contractile nature helps to explain the immediate and profound effects of stress on these symptoms, which anyone with PD will be able to relate to.
I've endeavoured to reduce symptoms through various movement and relaxation therapies over these past couple of years, not only improving my mobility, but also improving my proprioception and interoception (senses of my own body), and in doing so my experience/awareness of my symptoms has changed/sharpened, as I've begun to reconnect brain and body. It is also worth noting that important nerve endings which give us a sense of where our body parts are, and how these parts are moving, are also to be found in the fascia, because the resulting proprioceptive senses are atrophied or broken in people with PD.
Prior to learning about fascia, I would attempt to describe how it felt to me when I was very symptomatic with my rigidity dominant form of PD, by relating that it felt as if every muscle in my body was being clenched as hard as possible - and then just being stuck like that. Yet that has never felt quite right as an explanation for how it really feels. Somehow, the symptoms feel much more "surface" than just deep muscular. After learning more about fascia it became clear to me that my symptoms do feel as if something is happening in the connective tissue surrounding the muscles too. Indeed, when I learned that the nerve endings responsible for pain signals to the brain are embedded in the fascia, and that fascia contracts/stiffens/dehydrates in response to stress/threat, a piece of the jigsaw seemed to fall into place.
So, before looking further at some of the things which can go wrong with fascia, especially through prolonged chronic stress, I would like to go through some of my specific experiences and explain why I believe that "PD is in the fascia too" does fit.
Indeed, I had an extreme experience which helps inform things from my perspective, which occurred when I was hospitalized due to a severe and prolonged crisis,
MY HOSPITALIZATION WITH PARKINSON'S DISEASE.
During this time, my whole body became extremely stiff and rigid, such that I could no longer move at all. When I was in the hospital, for example, doctors would lift and bend my limbs to test reflexes and assess rigidity, but once they let go of a limb, it would remain in mid-air in the position the doctor had last placed it in - it was as I was an action figure that can be put into various poses. Thus, if a doctor raised my arm and bent it at the elbow and then let go, the arm would stay put in that position. For the arm to go back down on the bed, the doctor would have to physically press it down into the bed quite hard.
Yet, as the doctors manipulated me, it did not feel like each muscle was being activating and then cramping in place, nor did it feel like my muscles were straining against gravity to keep my arm aloft, and no apparent effort was involved. If I now try to imagine instead what would happen if my fascia had dried out completely or had become a very thick sticky substance and unable to flow, such that my skin would no longer slide against muscles, and muscle fibers would not be able slide or share loads, this then describes my experiences better. Imagining my fascia becoming plastic matches the experience of feeling like an action figure too.
As a second example, like many people with PD, my breathing is very shallow when I'm "off", and it is very hard to force deep breathing, and attempting to can actually be more triggering and make me freeze up worse. How I experience this is that the skin around my abdomen feels very tight when I try to expand my belly through breathing in. While the muscles feel tight and stiff too, this seems secondary, and I don't experience this as muscle "cramp" per se.
I also had a real "ah ha" moment about this while reading the book, which explained that the part of the fascia covering the stomach/abdomen is formed from a single sheet called an "aponeurosis".
This abdominal aponeurosis or "rectus sheath" covers the very area which feels tight when I am symptomatic, and feels more tight the more poorly I am, resulting in more restricted breathing, which can be very frightening when I am left to feel I can hardly breathe at all. This can lead to panic, which then increases the physical restriction, in a horrible feedback loop. For me, then, the concept that this abdominal sheet of fascia is constricting/tightening when the dopamine replacing PD drugs wear off, matches and explains my experience well.
We can also glean from the picture that, since the fascial net everywhere is connected to the abdominal sheet, its constriction inwards will have knock on effects to the rest of the "catsuit" and may cause tightening and pain elsewhere. For example, it is easy for me to visual that the abdominal tightening will pull downwards on the top of my shoulders, where most of my pain is, and result in the sensation that I am being pulled/pushed down to the floor (as if gravity has been increased) through my shoulder tops whenever I try to stand up against the PD.
It is interesting to note that other sheet like fascial regions exist between the ribs, on the back, on top of the head (the scalp) and on the palms of the hand and soles of the feet, and to imagine what would happen if each of these constricts, and match this to other common PD symptoms, such as curling up of the hands and feet.
Problems in the Fascia
According to the book cited above, the health of fascia is related to the structure and direction of the network of fibers. Very healthy fascia has a textile like weave and pattern to it, forming a lattice like structure and the fibers themselves have a nice waviness or "crimp" to them. On the other hand, problem areas of fascia lose the directonality of the fibers, which also lose their crimp, and the fascia then becomes a tangled mess of collagen fibers. This is nicely shown in the illustration from the book.
Tangled and unhealthy fascial structures can arise simply from immobility/sedentary lifestyles, poor posture (e.g. sitting in front of a computer too long), repetitive motions, the body being overtense or putting itself into threat response patterns for too long (i.e. chronic stress and trauma), and also from poor healing of physical injury. The point that fascia can “scar” and become problematic after an injury is important, since from talking with very many people with PD around the world in regards to their background histories before diagnosis, I have found that very many of us have had some form of injury to the neck, shoulders, back, hips, knees or feet, whether through accident, car crashes or surgery, in the years prior to diagnosis.
I believe it is possible to visibly observe that the fascia is problematic in people who have been immobile through PD for a long time, and this can be especially apparent by looking at the lower legs, which can often appear to have a shiny, plastic look, and have become hairless. It certainly doesn't require trained hands to feel that something is wrong in the fascia too in the bodies of people with PD, again especially in the lower part of the leg, which feel strangely solid and unyielding.
Pinch Points and Bottle Necks
It is easy to imagine that tangled messes of fibers would prevent the flow of the liquid part of the fascia gel, so will be more plastic than elastic, but also have negative effects on other structures and fluids passing through the fascia, such as blood vessels, lymph and nerve fibers. According to
Fascial plasticity – a new neurobiological explanation,
"This stimulated a German neurosurgeon to conduct a clinical study. They studied these fascial perforation points in patients suffering from chronic shoulder–neck or shoulder–arm pain. They found that the perforation points in these patients showed a peculiar anomaly. The perforating vessels were ‘strangled’ together by an unusually thick ring of collagen fibers around them, directly on top of the perforation hole."
Indeed, since the fascia contains free nerve endings responsible for pain signals, it seems clear that places in the body with chronic fascia problems may be associated with chronic pain. Furthermore, since the fascia tightens, contracts, congeals or dehydrates as part of preparedness of the body to react to threats, acute stress can rapidly make the chronic knotting and tangling worse and tighter, and more permanent, increasing blockage ratios and pain. This would help explain why acute stress visibly makes the physical symptoms of PD much worse.
These issues of the fascia make me wonder if some of the dystonia in my right neck and shoulder, which comes back whenever my PD meds wear off (several times a day), currently by far my most limiting remaining symptom, also has some involvement with connective tissue tightening. Indeed, since the neck contains many muscles and structures there is lots of fascia separating them, and hence a lot of possibilities for things to go awry. This can be clearly seen in the diagram below.
These anatomical structures in the neck really piqued my interest, especially all the fascial compartments. Clearly, there a lot of opportunities for fascial tangling, constriction or de-hydration to cause problems in the neck. Indeed, one feature I found very noteworthy is the “Cartoid Sheath”:
"The carotid sheath is an anatomical term for the fibrous connective tissue that surrounds the vascular compartment of the neck. It is part of the deep cervical fascia of the neck, below the superficial cervical fascia meaning the subcutaneous adipose tissue immediately beneath the skin.
“The four major structures contained in the carotid sheath are: the common carotid artery as well as the internal carotid artery (medial); internal jugular vein (lateral); the vagus nerve (CN X) (posterior); the deep cervical lymph nodes.”
“The carotid artery lies medial to the internal jugular vein, and the vagus nerve is situated posteriorly between the two vessels. In the upper part, the carotid sheath also contains the glossopharyngeal nerve (IX), the accessory nerve (XI), and the hypoglossal nerve (XII), which pierce the fascia of the carotid sheath.
Constriction of the fascia forming the Cartoid Sheath might cause Vagus Nerve dysregulation (nerve pinching). I cannot overstate the importance of this direct link between fascia and Vagus Nerve, since my perspective is that dysfunction of the Vagus Nerve and related Parasympathetic Cranial Nerves is central to Parkinson’s Disease, see:
THE DORSAL VAGUS NERVE AND PARKINSON'S DISEASE,
THE NERVOUS SYSTEM AND PARKINSON'S DISEASE,
THE CRANIAL NERVES AND PARKINSON'S DISEASE.
Furthermore, fascial constriction here could result in oxygen supply to the brain issues, see
LACK OF OXYGEN TO THE BRAIN IN PARKINSON'S DISEASE,
and immune responses and problems with lymph drainage of brain too resulting in toxin build up. Again, this matches my own experience and helps explain why being in a seated position is by far the most uncomfortable for me. I can't actually sit for very long at all when "off", as it feels like the blood supply to my head is being cut off and I freeze even more. This causes severe brain fog, freezing up, anxiety and my cranial nerves going offline, such as my eyes becoming unfocussed and unblinking, my ability to speak going. If I am stressed at the time, it is much worse. There is another very vicious circle with PD in that getting stressed about the pain/symptoms rapidly makes the pain/symptoms worse, and again this may perhaps be due to the resulting fascial tightening with stress.
Furthermore, some sort of problem with the fascia in the neck is often visible in people with PD, where the structures stand out and are very prominent, an example of which is shown in the photo below.
What Can We Do?
Firstly, just as stress tightens the fascia, relaxation can bring relief. So in the short time, this is one reason why stress management and learning relaxation techniques, especially meditation, is vital for coping with PD.
Longer term, all is not lost, however, because the book cited at the top of this article also explains that fascia contains special cells callled "fibroblasts" which not only lay down new collagen fibers but also gobble up old ones. It is therefore possible for fascial history to be rewritten over time. This requires the proper stimulation of these cells, whether by appropriate self-motivated or self-induced movement therapies (e.g. types of yoga, dance, exercise, sports, etc) or hands-on therapies (various 'myofascial release' modalities - see the book for a partial list of these).
On the other hand, fascia problems are likely to get worse through a lack of movement. Tangled fibres areas are likely to grow and new problem areas may be seeded, if the response to a movement disorder or pain is to become even more sedentary or immobile, or to constantly protect the painful area. In this sense, it is easy to see why Parkinson's Disease can therefore be "degenerative", since lack of dopamine results in a lack of motivation to move, which just make it harder and even more of an effort to mobilize, which means the fibroblasts get even less stimulation, resulting in the build up of more problem fascia, causing pain, rigidity and stiffness to worsen and spread. Conversely, this is one reason why very regular exercise and movement therapies are proving so beneficial to the long term prognosis for people with PD and related conditions, because it helps stimulates the fibroblasts into adapating the fascia to the movement signals, reversing some of the initial problem,